Drug Resistance: Antineoplastic
Antineoplastic Resistance
Antineoplastic resistance is a well-known phenomenon --- the ability of resistance of neoplastic cells to survive and grow during the anti-cancer pharmaceutical treatments. There are two general causes of antineoplastic therapy failure; one is intrinsic resistance that exists before drug treatment, resulting in resistance of cancer cells; the other is acquired resistance induced after drug exposure based on the cancer cell heterogeneity.
Intrinsic resistance, also known as cell-autonomous resistance, is the innate resistance that exists before being exposed to drugs. It involves pre-existing (inherent) genetic mutations and heterogeneity of tumors. Acquired drug resistance refers to a non-cell-autonomous mechanism, which is based on the treatment process related to changes in the tumor microenvironment after treatment. The tumor microenvironment mediated drug resistance is associated with tumor cells and their pericellular matrix. The development of antineoplastic drug resistance has limited the clinical efficacy and effectiveness of the antineoplastic treatment.
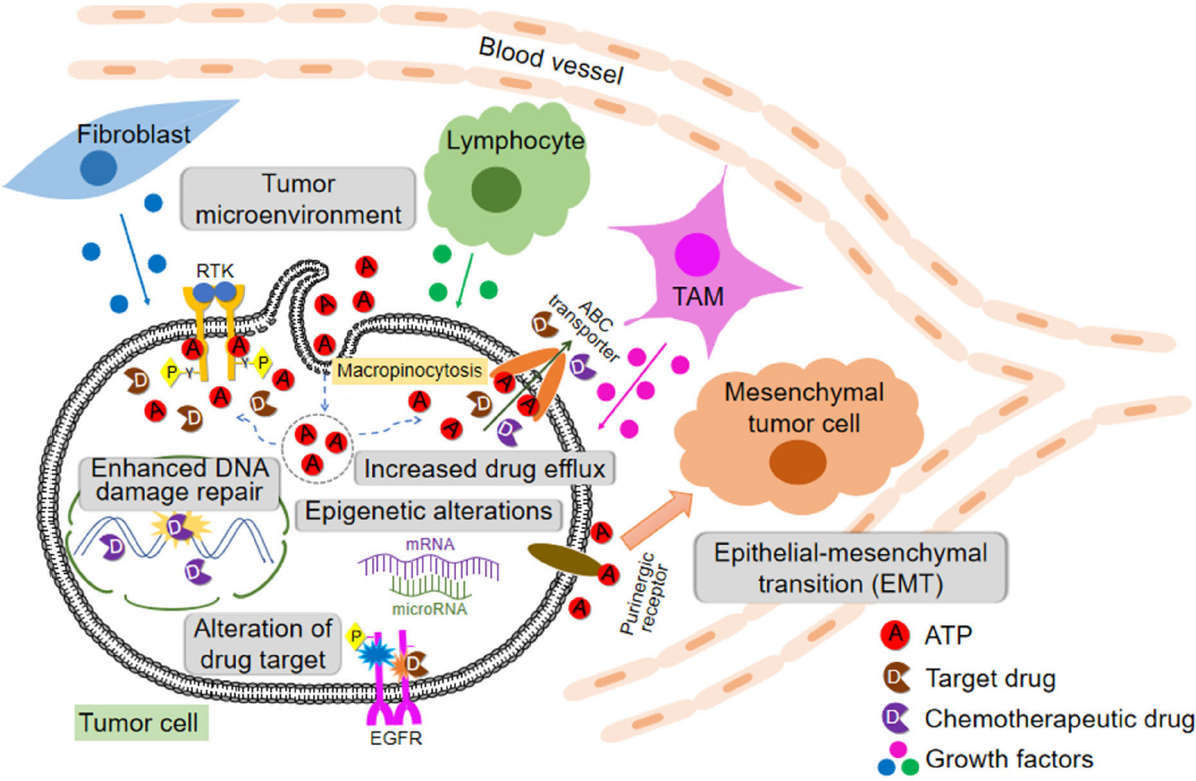 Fig.1 Antineoplastic resistance.1
Fig.1 Antineoplastic resistance.1
Major Types of Antineoplastic Resistance
- EGFR tyrosine kinase inhibitor resistance
- Platinum drug resistance
- Antifolate resistance
- Endocrine resistance
Mechanisms of Antineoplastic Drug Resistance
-
Cancer cell heterogeneity
Different populations of cancer cell heterogeneity possess inherent characteristics, including genetic mutations and epigenetic changes (miRNA, transcriptomic, and proteomic heterogeneity). The genetic mutations include mutations, gene amplifications, deletions, chromosomal rearrangements, transposition of the genetic elements, translocations, and microRNA alteration. Antineoplastic drugs only kill drug-sensitive cells. During the treatment of cancers, some resistant cancer cells can survive, mutate, and propagate, eventually creating new heterogeneous tumors and causing cancer relapses over time.
-
Tumor microenvironment
The tumor microenvironment includes various types of cells and extracellular components, such as normal stromal cells, extracellular matrix, cytokines, growth factors, and signaling molecules. The dynamic changes of the tumor microenvironment in the course of treatment mediates tumor progression and affects treatment efficacy. The tumor microenvironment-driven significant non-cell-autonomous mechanism of resistance is a critical mechanism that can resist various types of antineoplastic drugs, causing the failure of anti-cancer treatment.
-
Epigenetic mechanisms
Epigenetic modification plays an essential role in antineoplastic drug resistance and causes resistance to cancer treatment. Two main types of epigenetic changes are DNA methylation and histone methylation/acetylation. DNA methylation is an important epigenetic process to silence individual genes effectively. Specific histone modifications, such as acetylation and deacetylation, could regulate gene expression and alter chromatin formation. Overall, epigenetic alterations such as oncogenes activated through hypermethylation and tumor suppressors silenced through hypermethylation are recognized as the causes of drug resistance in different kinds of cancers.
-
Others
Other mechanisms of cancer cells reduce efficacy of drugs by reducing drug accumulation, enhancing drug efflux, enhancing DNA damage repair, eliminating pathway defects, altering target molecules and metabolism, and impairing apoptosis.
Overcoming Antineoplastic Drug Resistance
Due to the differences of target multiple driver genes, combination and personalized treatment regimen should be the best treatment option to consider and develop because it prevents the increasing drug resistance and is more effective than any drug used alone. To avoid potential pre-existing drug resistance, biochemical analyses should be performed before the treatment of cancer; therapeutic plans need to be adjusted accordingly after the acquired drug resistance is developed. Moreover, advances in the development of targeted therapies and tumor microenvironment targeted treatments can regulate the efficacy and effectiveness of antineoplastic drugs, providing new strategies for combinations of antineoplastic drugs to prevent, delay, or even overcome drug resistance.
Reference
- Wang, Xuan et al. “Drug resistance and combating drug resistance in cancer.” Cancer drug resistance (Alhambra, Calif.) vol. 2,2 (2019): 141-160. doi:10.20517/cdr.2019.10. Distributed under Open Access license CC BY 4.0, without modification.
For research use only. Not intended for any clinical use.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.

