Maturity Onset Diabetes of the Young Overview
Introduction of Maturity Onset Diabetes of the Young
Maturity Onset Diabetes of the Young (MODY) is an inherited type of diabetes mellitus caused by a change in one of eleven genes. MODY is very rare compared with Type 1 and Type 2 diabetes, around 2-5% of all non-insulin-dependent diabetes. In fact, it’s estimated that around 90% of people with MODY are mistakenly diagnosed with type 1 or type 2 diabetes in the beginning. There are eleven types of MODY caused by mutations in eleven different genes. There are several common forms of MODY, including MODY1, MODY2, MODY3, MODY4, MODY5, MODY6. MODY1 is caused by a change in the hepatocyte nuclear factor-4-alpha gene (HNF4A) on chromosome 20. MODY2 is caused by a mutation in the glucokinase gene (GCK) on chromosome 7. MODY3 is resulted from a mutation in the hepatic transcription factor-1 gene (TCF1) on chromosome 12q24.2. MODY4 is caused by the mutation in the insulin promoter factor-1 gene (IPF1) on chromosome 13q12.1. MODY5 is caused by the mutation in the gene encoding hepatic transcription factor-2 (TCF2) on chromosome 17cen-q21.3. MODY6 is caused by the mutation in the gene encoding neurogenic differentiation 1 (NEUROD1) on chromosome 2q32.
Similar to other patients with diabetes, people with MODY have trouble regulating their blood sugar levels. For patients with type 1 diabetes, their pancreas cannot make and release enough insulin. People with type 2 diabetes, on the other hand, produce enough insulin but their bodies are unable to respond to it effectively (a condition known as insulin resistance). Type 2 diabetes is usually associated with being overweight, but that is not true of type 1 diabetes or MODY. However, an obese person with a MODY gene mutation may develop symptoms of diabetes sooner than someone of normal weight. Except for affecting regulating blood sugar levels, MODY also results in complications throughout the body, including an increased risk of heart and vascular disease, kidney disease, and blindness. MODY is more likely to affect adolescents and young adults, but it can occur at any age.
Overview of MODY pathways
Main Signaling Pathway in Maturity Onset Diabetes of the Young
Diagnosis of Maturity Onset Diabetes of the Young
According to the recent diagnostic criteria, MODY is characterized by an onset before 25 years of age, the presence of diabetes in two consecutive family generations, the absence of β-cell autoantibodies, and preserved endogenous insulin secretion with a serum C-peptide level of >200 pmol/L. These diagnostic criteria have been well accepted for distinguishing MODY from type 1 and type 2 diabetes. The first step in the whole diagnostic process is going through a blood sugar test. Blood tests can help doctors determine which kind of diabetes patients have. For instance, antibodies attack the pancreas if someone has type 1 diabetes, but people with MODY do not have these antibodies. Doctors will also look for some typical signs in patients’ blood tests that indicate whether they have insulin resistance. Insulin resistance does not occur in non-obese people with MODY; it is present in obese people with MODY. However, these tests may be difficult to tell whether an obese person has type 2 diabetes or MODY because the great majority of obese people with diabetes have type 2 diabetes. Therefore, it is necessary to do the genetic test. Nonobese subjects with hyperglycemia, no evidence of -cell autoimmunity, and preserved -cell function are candidates for genetic testing. This type of testing will determine the exact type of MODY, and also can be done before a patient has any symptoms. If a mutation in one of the MODY genes is found, this indicates that type 1 or type 2 diabetes can be ruled out.
Targeted Therapy for Onset Diabetes of the Young
Based on different types of MODY, treatments are various. Losing weight can be helpful and better for patients with MODY. Furthermore, the treatment is primarily determined by the type of patients:
- MODY 1 and MODY 4. They are commonly treated with sulfonylureas, including glipizide (Glucotrol) and glyburide (Glynase Pres Tab, others). These drugs help the pancreas make more insulin. Furthermore, some people with MODY 1 and MODY 4 may need to take insulin.
- MODY 2. These patients require more exercise and a healthier diet rather than drugs or insulin therapy.
- MODY 3. In the beginning, this disease can be treated through diet. Over time, patients need sulfonylureas and then insulin.
- MODY 5. Patients need to take insulin to treat it. This rare form of MODY harms other organs and causes complications, such as kidney cysts or kidney failure.
- MODY 6. This type may occur later, around the age of 40. Patients have to get treated with insulin.
For research use only. Not intended for any clinical use.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.


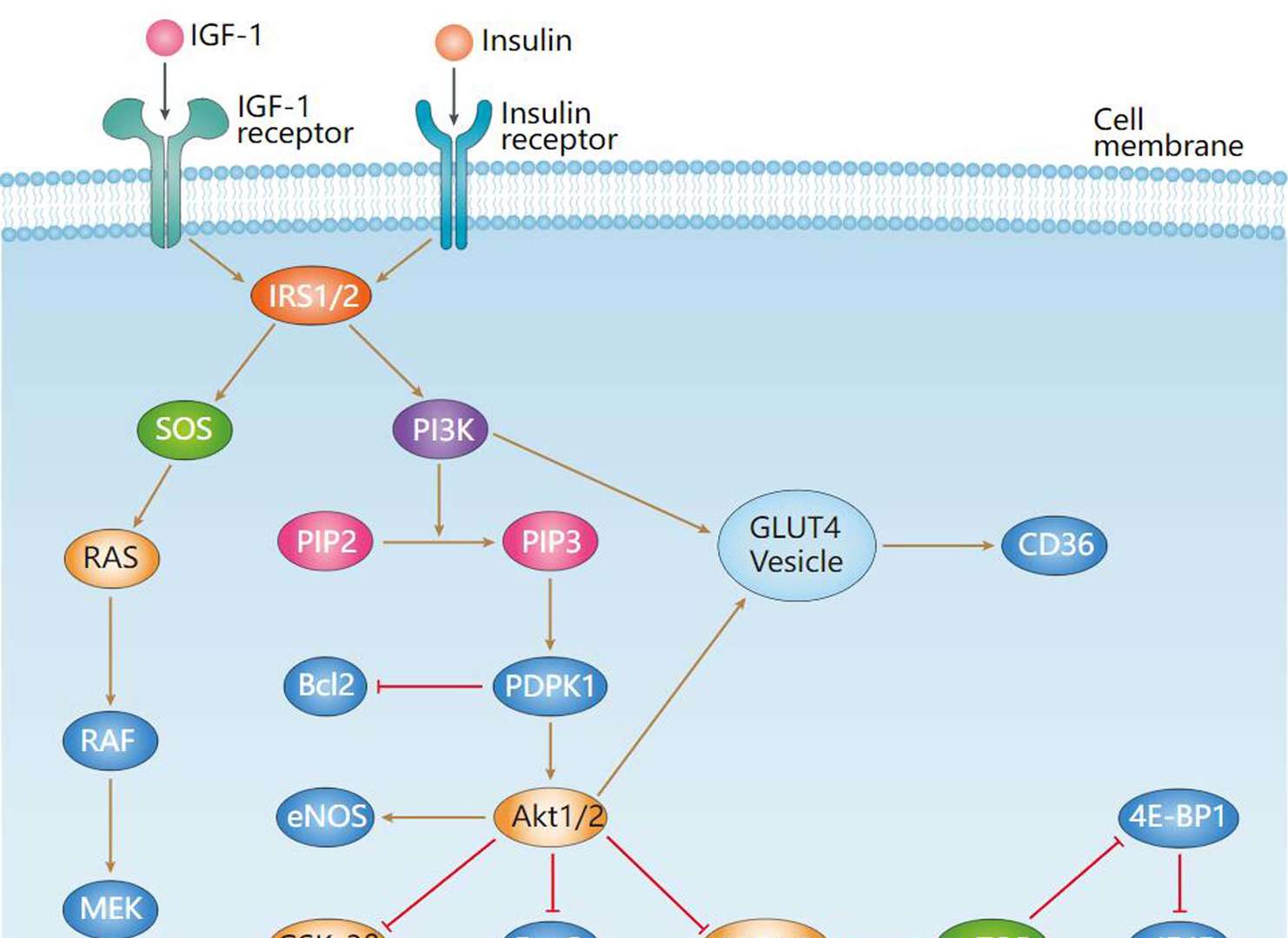 Insulin Signaling Pathway
Insulin Signaling Pathway