Rheumatoid Arthritis Overview
Rheumatoid arthritis (RA) is a chronic inflammatory disorder that can cause joint pain and damage throughout your body. As an autoimmune disorder, RA occurs when your immune system mistakenly attacks your own body's tissues. RA can affect several organs in the body, the joint symptoms of RA include joint pain, joint swelling, joint stiffness, and loss of joint function and deformities. These symptoms and signs happen during stages known as flares or exacerbations. Symptoms can vary from mild to severe. Everyone can get RA. Research studies suggest that this disorder is two to three times more common in women than in men, but men tend to have more severe symptoms. It usually occurs in middle age. But young children and the elderly also can get it. RA can affect everyone differently. For some, joint symptoms happen gradually over several years. In others, it may come on quickly. Some people may have RA for a short time and then go into remission, which means they don’t have symptoms. While new types of medications have improved treatment options dramatically, severe RA can still result in physical disabilities.
Main Signaling Pathways in Rheumatoid Arthritis
Diagnosis of Rheumatoid Arthritis
Firstly, undergoing an in-depth discussion of the problem with doctors about patients’ past and relatives, if someone in your family tree has RA, you may be more likely to have the disease. After the discussion, patients will have a thorough physical examination. The most important thing is to observe which joints are swollen. Specific finger and toe joints are usually inflamed in RA. But swelling and pain in larger joints like the shoulders or knees may also be a sign of RA. It's also important to find out how many joints are affected and how long they've been inflamed. During these tests, blood tests are employed to detect certain antibodies and signs of inflammatory response. But these tests only have limited usefulness for the early diagnostics because the results may vary for other reasons as well. It can be difficult to diagnose RA at an early stage because the symptoms are often very mild in the first few weeks and months, and may not be typical. Besides these tests, doctors also utilize imaging tests to confirm the condition. RA can cause the ends of the bones within a joint to wear down (erosions). An X-ray, ultrasound, or MRI (magnetic resonance imaging) scan can look for erosions.
Targeted Therapy for Rheumatoid Arthritis
RA is treated with both medication and non-drug approaches, such as physiotherapy. Physiotherapy and sports can help improve or maintain flexibility, strength and joint function. In terms of medications, it can decrease inflammation and help keep the disease from getting worse, relieve symptoms like pain and swelling, and help people move their joints more easily again, or at least maintain joint flexibility for as long as possible.
For research use only. Not intended for any clinical use.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.


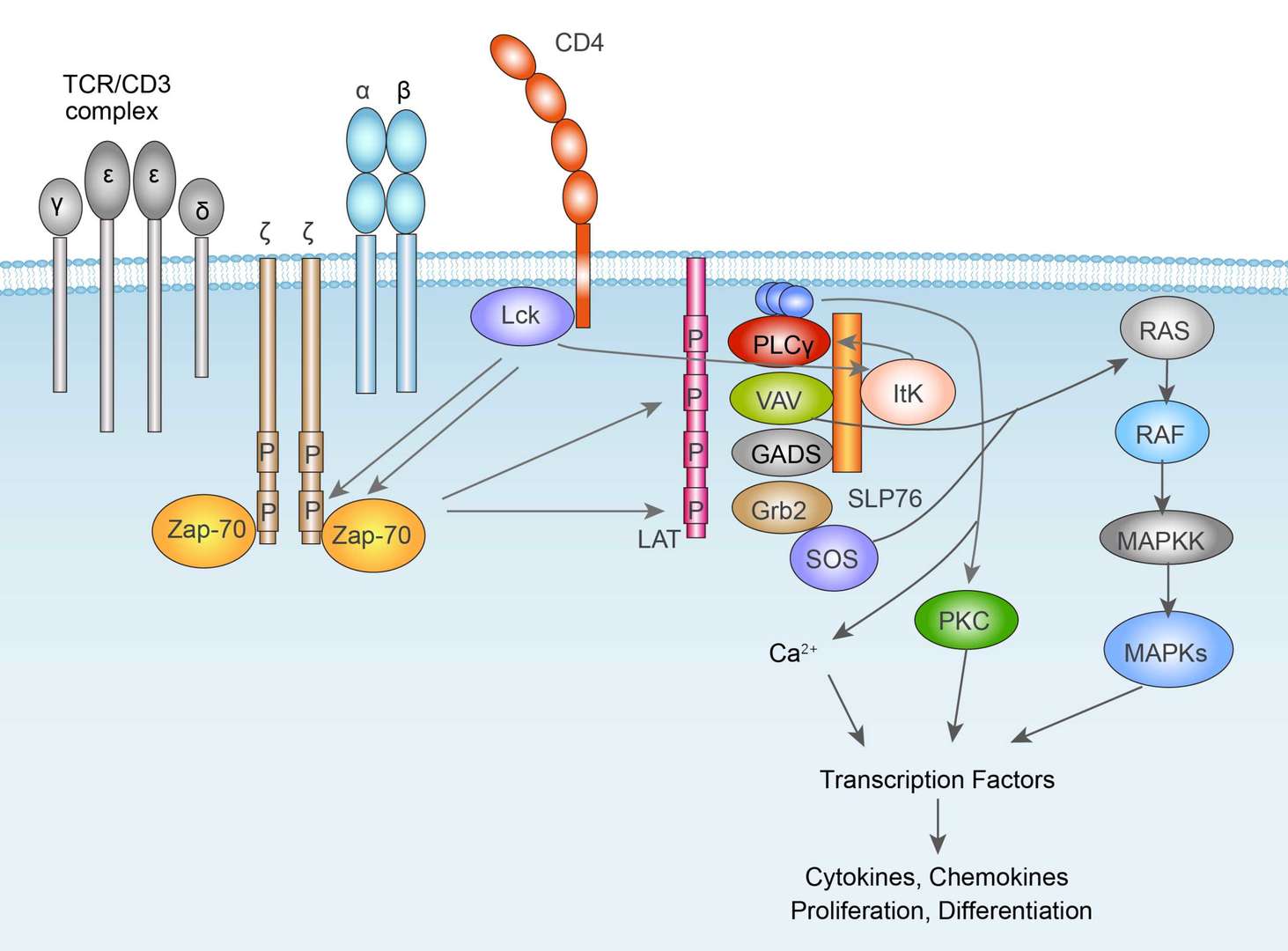 TCR signal pathway
TCR signal pathway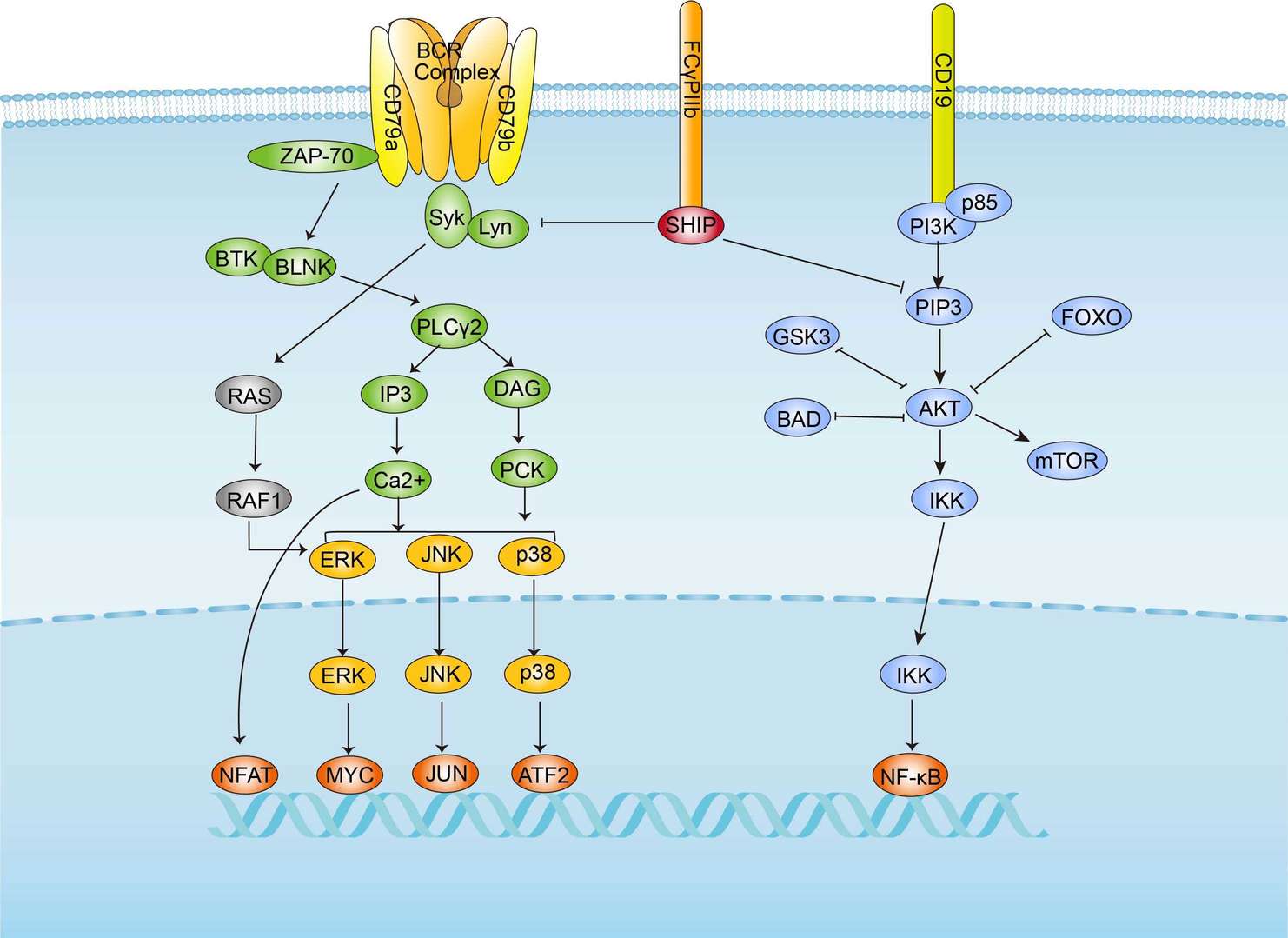 BCR signal pathway
BCR signal pathway